Rotator Cuff Tears
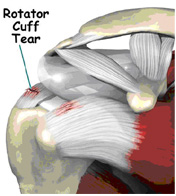
Rotator cuff tears are a common source of shoulder pain. The incidence of rotator cuff damage increases with age and is most frequently caused by degeneration of the tendon, rather than injury from sports or trauma.
Anatomy
The rotator cuff is a group of four muscles that surround the humeral head (ball of the shoulder joint). The muscles are referred to as the "SITS" muscles: supraspinatus, infraspinatus, teres minor, and subcapularis. The muscles function to provide rotation, elevate the arm, and give stability to the shoulder joint (glenohumeral joint). The supraspinatus is most frequently involved in degenerative tears of the rotator cuff. More than one tendon can be involved. There is a bursa (sac) between the rotator cuff and acromion that allows the muscles to glide freely when moving. When rotator cuff tendons are injured or damaged, this bursa often becomes inflamed and painful.
Pain, loss of motion, and weakness may occur when one of the rotator cuff tendons tears. The tendons generally tear off at their insertion (attachment) onto the humeral head.
Cause
The rotator cuff can be torn from a single traumatic injury. Patients often report recurrent shoulder pain for several months and a specific injury that triggered the onset of the pain. A cuff tear may also happen at the same time as another injury to the shoulder, such as a fracture or dislocation.
Most tears, however, are the result of overuse of these muscles and tendons over a period of years. People who are especially at risk for overuse are those who engage in repetitive overhead motions. These include participants in sports such as baseball, tennis, weight lifting, and rowing.
Rotator cuff tears are most common in people who are over the age of 40. The blood supply to the rotator cuff diminishes with age and transiently with certain motions and activities. The substance of the tendon itself degenerates over time. Because of the decrease in tendon blood supply, the body's ability to repair tendon damage is decreased with age; this can ultimately lead to a full-thickness tear of the rotator cuff.
Rotator cuff tear may often happen as a result of wear and tear. An extrinsic factor that can cause damage to the rotator cuff is the presence of bones spurs underneath the acromion. The spurs rub on the tendon when the arm is elevated; this is often referred to asimpingement syndrome. Combining this with a diminished blood supply, the tendons have a limited ability to heal themselves. These factors are at least partly responsible for the age-related increase in rotator cuff disease and the higher frequency in the dominant arm.
Younger people tend to have rotator cuff tears following acute trauma or repetitive overhead work or sports activity.
Symptoms
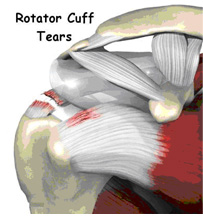
Some of the signs of a rotator cuff tear include:
- Atrophy or thinning of the muscles about the shoulder
- Pain when lifting the arm
- Pain when lowering the arm from a fully raised position
- Weakness when lifting or rotating the arm
- Crepitus or crackling sensation when moving the shoulder in certain positions
Symptoms of a rotator cuff tear may develop right away after a trauma, such as a lifting injury or a fall on the affected arm. When the tear occurs with an injury, there may be sudden acute pain, a snapping sensation and an immediate weakness of the arm. Symptoms may also develop gradually with repetitive overhead activity or following long-term wear. Pain in the front of the shoulder radiates down the side of the arm. At first, the pain may be mild and only present with overhead activities, such as reaching or lifting. It may be relieved by over-the-counter medication such as aspirin or ibuprofen.
Over time the pain may become noticeable at rest or with no activity at all. There may be pain when lying on the affected side and at night.
Diagnosis
Diagnosis of a rotator cuff tear is based on the symptoms and physical examination. X-rays, and imaging studies, such as MRI or ultrasound, are also helpful.
Physical examination includes looking for any tenderness or deformity including the Impingement sign . Range of motion of the shoulder is measured in several different directions and the strength of the arm is tested . We also check for instability or other problems with the shoulder joint.
We will also examine the neck to make sure that the pain is not coming from a " pinched nerve " in the cervical spine and to rule out other conditions, such as osteoarthritis or rheumatoid arthritis.
Plain X-rays of a shoulder with a rotator cuff tear are usually normal or show a small spur. For this reason , an MRI may be required to better visualize soft tissue structures such as the rotator cuff tendon .The MRI can tell how large the tear is, as well as its location within the tendon itself or where the tendon attaches to bone.
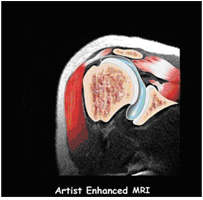
MRI Scan image shows a full-thickness rotator cuff tear within the tendon.
Rotator Cuff Tears and Treatment Options
Treatment recommendations vary from rehabilitation to surgical repair of the torn tendon(s). The best method of treatment is different for every patient.
The decision on how to treat rotator cuff tears is based on the patient's severity of symptoms, functional requirements, and presence of other illnesses that may complicate treatment.
Nonsurgical Options
Non Surgical treatment typically involves activity modification (avoidance of activities that cause symptoms). This treatment can provide pain relief and improve the function of the shoulder of a rotator cuff tear in approximately 50% of patients
Nonsurgical treatment options may include:
- Rest and limited overhead activity
- Use of a sling
- Anti-inflammatory medication
- Steroid injection
- Strengthening exercise and physical therapy
We recommend nonsurgical treatment for patients who are most bothered by pain, rather than weakness, because strength does not tend to improve without surgery.
Disadvantages of nonsurgical treatment are
- Strength does not improve
- Tears may increase in size over time
- Patient may need to decrease activity level
Surgical Intervention and Considerations
Surgery is recommended if
- Nonsurgical treatment does not relieve symptoms
- The tear has just occurred and is very painful
- The tear is in the shoulder of the dominant arm of an active person
- If maximum strength in the arm is needed for overhead work or sports
The type of surgery performed depends on the size, shape, and location of the tear. A partial tear may require only a trimming or smoothing procedure, called a debridement. A complete tear within the thickest part of the tendon is repaired by suturing the two sides of the tendon back together. If the tendon is torn away from where it inserts into the bone of the arm (humerus), it is repaired directly to bone.
During surgery to repair a torn rotator cuff , if there are bony spurs , they are removed along with a part of the acromion bone called Acromioplasty . Other conditions such arthritis of the AC joint or tearing of the biceps tendon may also be addressed.
The three commonly used surgical techniques for rotator cuff repair are:
- Open repair
- Mini-open repair
- All-arthroscopic repair
Each of the methods available has its own advantages and disadvantages; all have the same goal�getting the tendon to heal to the bone. The choice of surgical technique depends on several factors, including the surgeon's experience and familiarity with a particular procedure, the size of the tear, the patient's anatomy, the quality of the tendon tissue and bone, and the patient's needs. Regardless of the repair method used, studies show similar levels of pain relief, strength improvement, and patient satisfaction.
We use special fasteners to anchor the rotator cuff to the humerus. During the procedure, we make small drill holes into the humerus. A suture anchor is punched down inside the drill hole. By tugging on the suture, the fastener becomes anchored to the bone. The tendon is then sewn together and stitched to the humerus by looping sutures over the edge of the rotator cuff.
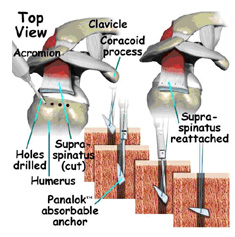
Many surgical repairs can be done on an outpatient basis
Surgical Procedure
Open Repair
Open repair is performed without arthroscopy. We make an incision over the shoulder and detach the deltoid muscle to gain access to and improve visualization of the torn rotator cuff . We will usually perform an acromioplasty (removal of bone spurs from the undersurface of the acromion) as well. The incision is typically several centimeters long. Open repair was the first technique used to repair a torn rotator cuff; over the years, the introduction of new technology and improved surgeon experience has led to the development of less invasive surgical procedures. Although a less invasive procedure may be attractive to many patients, open repair does restore function, reduce pain, and is durable in terms of long-term relief of symptoms.
In this photograph, the typical incision size for a mini-open rotator cuff repair is shown in black on a patient''s left shoulder.
As the name implies, mini-open repair is a smaller version of the open technique. The incision is typically 3 cm to 5 cm in length. This technique also incorporates arthroscopy to visualize the tear and assess and treat damage to other structures within the joint . Arthroscopic removal of spurs (acromioplasty) avoids the need to detach the deltoid muscle. Once the arthroscopic portion of the procedure is completed, we proceed to the mini-open incision to repair the rotator cuff. Mini-open repair can be performed on an outpatient basis. Currently, this is one of the most commonly used methods of treating a torn rotator cuff; results have been equal to those for open repair. The mini-open repair has also proven to be durable over the long-term.
All-Arthroscopic Repair
Arthroscopic photographs of a rotator cuff tear (left) and the final repair (right). This was performed all-arthroscopically. Sutures were used to reattach the tendon back to bone .
This technique uses multiple small incisions (portals) and arthroscopic technology to visualize and repair the rotator cuff. All-arthroscopic repair is usually an outpatient procedure. The technique is very challenging, and the learning curve is steep. It appears that the results are comparable to those for mini-open repair and open repair.
Results
After rotator cuff repair, 80% to 95% of patients achieve a satisfactory result, defined as adequate pain relief, restoration or improvement of function, improvement in range of motion, and patient satisfaction with the procedure.
Surgical techniques for rotator cuff repair have progressed to more minimally invasive procedures. Each step toward less invasive surgery has benefited the patient by:
- Decreasing pain from surgery
- Decreasing postoperative stiffness
- Decreasing surgical blood loss
- Decreasing length of stay in the hospital
Each technique has similar results in terms of satisfactory relief of pain, improvement in function, and patient satisfaction. Less invasive surgery results in an easier rehabilitation process and less postoperative pain.
Improvement in pain, function, and strength typically occurs over a 4 to 6 month period following the procedure.
Complications
Like all surgeries , rotator cuff repair surgery has some complications seen in 2-3% of patients . These include nerve injury , infection , deltoid detachment , stiffness & tendon re-tear which can be minimised by meticulous surgical techniques .
Rehabilitation
Following rotator cuff surgery, therapy progresses in stages . Initially, the repair needs to be protected until adequate healing of the tendon to bone occurs. For this reason, most patients use a sling for the first 4 to 6 weeks after surgery and are instructed to limit active use of the arm during this period. Passive range-of-motion exercises are begun with a therapist pendulum exercises may be taught as well. Progressive strengthening and range-of-motion exercises continue during the next 6 to 12 weeks. Most patients have a functional range of motion and adequate strength by 4 to 6 months after surgery.
A strong commitment to rehabilitation is important to achieve a good surgical outcome. We will examine the outcome to advise when it is safe to return to overhead work and sports activity.
Summary
The incidence of full-thickness rotator cuff tears increases with age; however, tears are not always painful. Tears can be managed successfully with nonsurgical treatment in 50% of patients. Pain and range of motion will improve with nonsurgical management, but strength will not. Large tears, significant weakness, and an acute traumatic event are possible causes of poor outcome from nonsurgical management.
Surgical repair results in pain reduction and improved function and strength in more than 80% of patients. About 2-3% of surgeries can result in complications. Surgical procedures to repair a torn rotator cuff have become increasingly less invasive. Minimally invasive procedures are less painful and have less blood loss, shorter hospital stays, and a generally easier rehabilitation period. Although less invasive procedures are more attractive, they are often more difficult for the surgeon to perform and require an experienced surgeon for best results. Lastly, all repair methods appear equal in outcomes when the surgery is performed well.
